|
| Abstract:
Background: Vitiligo is a common idiopathic acquired depigmentation disorder that can be classified into segmental and non- segmental varieties. Reports on the epidemiology of vitiligo in The Middle East comparing the two varieties are few.
Aim: To define and analyse the clinical profiles of vitiligo in Al- Minya, Egypt as a representative of The Middle East highlighting the difference between the segmental and the non- segmental varieties.
Methods: This study included 1100 patients with vitiligo presented to the Department of Dermatology at Al- Minya University Hospital and Al- Minya Centre for Vitiligo Phototherapy and Surgery over a period of 4 years.
Results: Of the 1100 Egyptian vitiligo patients, females represented 78.9% of patients in the non- segmental vitiligo group and 55.5% in the segmental vitiligo group. The commonest type of vitiligo was the generalized [58.2%] followed by the focal [34.9%] and then the segmental type [6.9%]. The mean age at onset of the segmental and non- segmental groups were 8.6 and 21.8 years and the mean age at presentation were 17.3 and 28.07 years respectively. The commonest affected site in the non- segmental group was the limbs while in the segmental group it was the face. Positive family history, detection of associated disorders and side effects of previous therapy were reported in the non- segmental group only.
Conclusions: The mean age at onset and at presentation, sex predilection, positive family history and associated diseases are significantly different between the segmental and non- segmental Egyptian vitiligo groups. These findings stresses the view that segmental and non- segmental vitiligo as two completely different subtypes. Introduction:
Vitiligo is a common idiopathic acquired depigmentation disorder, affecting 1-2% of the world population.[1] Clinically, several types of vitiligo are distinguished according to the distribution of the achromic lesions. One or more lesions in a dermatomal pattern are characteristic for segmental vitiligo (SV) while this segmental distribution is absent in non segmental vitiligo (NSV). The latter variety includes both the focal type and the generalized type.[2] The SV usually has an early onset and spreads rapidly in the affected dermatomal area then persist unchanged for the rest of the patient's life.[3] On the other hand, NSV could occur at any age.[4] Some authors suggested a different pathogenesis for each.[4,5,6] There is a paucity of well- designed epidemiological studies on vitiligo [7] and studies that categorise vitiligo into types are few. Aim of the work:
To define and analyze the clinical profiles of vitiligo and to identify the relationship between them, highlighting their association with systemic and dermatologic diseases. Patients and methods:
Patients: A prospective study included 1100 vitiligo patients who attended the Department of Dermatology at Al- Minya University Hospital and Al- Minya Center for Vitiligo Phototherapy and Surgery over a period of 4 years. Data complied were sex, age at initial visit, age at onset, affected sites, dermatomal distribution, family history, the side effects of previous therapy for vitiligo, and any associated medical diseases or skin disorders. The types of vitiligo were categorized as segmental, focal or generalized.
Ethical consideration: Each patient or guardian signed a written consent form to be included in the study and to be photographed if needed.
Statistical analysis: Data were analyzed by the Statistical Package for the Social Sciences (SPSS for windows version 11.0, SPSS Inc.). Descriptive statistics in the form of the frequency, percentage, range, mean and standard deviation were calculated. Comparison between patients and controls was done by the Student's t-test for paired observations. Results:
A total number of 1100 patients were enrolled in this study. Patients were classified according to their types of lesions into two groups: segmental vitiligo (SV) group {Fig 1} and non- segmental vitiligo (NSV) group {Fig 2}.
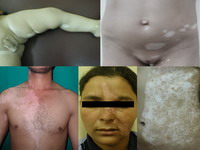 | Fig 1: Segmental vitiligo lesions: lesions affect different body sites |
|

Fig
2: Non- segmental vitiligo lesions:
(A): Focal lesion on forearm,
(B): generalized trunk lesions,
(C and D): lesions on feet of the same
patient in B.
-Note the symmetricity in B, C and D |
|
The SV groups included 76 patients (6.9%) and the NSV group included 1024 patients (93.1%). The NSV group was further subdivided into focal type (384 patients representing 34.91%) and generalized type (640 patients representing 58.18%). No significant difference was found between males and females, neither in the whole study nor in the NSV group. On the other hand, females were predominant in the SV group (Table 1).
|
|
Males |
Females |
|
SV |
16 (21.1%) |
60 (78.9%) |
|
NSV |
456 (44.5%) |
568 (55.5%) |
Table 1: Sex distribution in vitiligo
groups
Age at onset and age at presentation: The mean age at onset and mean age at presentation were significantly earlier in the SV group than the NSV group (P value <0.0005). (Table 2)
|
|
Age
at onset |
Age
at presentation |
|
Minimum |
Maximum |
Mean +
SD |
Minimum |
Maximum |
Mean +
SD |
|
NSV |
1 |
57 |
21.08 +
11.39 |
5 |
62 |
28.07 +
12.66 |
|
SV |
1 |
21 |
8.6 + 6.6 |
1 |
30 |
17.3 + 7.66 |
Table 2: Age of onset and age at
presentation in vitiligo groups
Sites of involvement: In the NSV group, the limbs were the commonest affected site followed by the acral areas then the trunk and the least affected site was the face while in the SV group, the face was the commonest site affected followed by the limbs and then the trunk. The acral areas were not affected in any of the patients in this group
(Table 3).
|
|
Limbs |
Trunk |
Face |
Acral Areas |
Affection of >one site |
|
SV |
28 patients |
20 patients |
40 patients |
0 |
12 patients |
|
(36.84%) |
(26.31%) |
(52.63%) |
(0%) |
(15.78%) |
|
NSV |
568 patients |
400 patients |
356 patients |
404 patients |
548 patients |
|
(55.46%) |
(39.06%) |
(34.76%) |
(39.45%) |
(53.52%) |
Table 3: Sites of involvement and
extension of lesions
Extension of the lesions: Affection of more than one side was detected in 53.52% of the NSV patients and in only 15.8% of the SV patients
(Table 3). Family History: Ninety- nine patients, constituting 9% of the whole study group and 9.67% of the NSV group, reported a positive family history of the disease while none of the patients of the segmental group reported any family history which was statistically significant. (P value = 0.002)
Side effects of previous therapy: All the side effects were reported in the NSV group {Fig 3}. The previous use of topical or intra- lesional steroids resulted in localized areas of atrophy in 48 patients (4.4% of the study group and 4.7% of the NSV group) and telangiectasia in 8 patients (0.7% of the study group and 0.78% of the NSV group). Other side effects of previous therapy detected included failed medical tattoo in 12 patients (1.1% of the study group and 1.17% of the NSV group) and post- psoralens hyper-pigmentation in one patient (0.09% of the study group and 0.1% of the NSV group).
 Fig
3: Adverse effects of previous therapy:
(A) telangiectasia
(B) atrophy and
(C) failed medical tattoo. |
|
Associated medical diseases:
These were in the form of diabetes mellitus in 36 patients (3.27%) and hyperthyroidism in three patients (0.27%). Meanwhile, if these figures are related to the NSV group they will be 3.51% and 0.29% respectively. None of the SV patients reported any associated autoimmune diseases.
Associated skin diseases: Lichen planus was detected in 20 patients (1.81%) {Fig 4}, Halo
nevi in 16 patients (1.45%), alopecia areata in 12 patients (1.09%) {Fig 5}, psoriasis in 8 patients (0.72%) {Fig 6} and capillary
hemangioma {Fig 7}, squamous cell carcinoma {Fig 8} and keloid {Fig 9} were associated with vitiligo in one patient each (0.09%). These figures will be 1.95%, 1.56%, 1.17%, 0.78%, and 0.1% respectively on considering the NSV group. Again, none of the SV patients reported any associated skin disorders.
 |
Fig 4: Vitiligo associated with lichen planus.
Note that the LP lesions are erythematous when involving
the vitiliginous skin and violaceous elsewhere. |
|
 |
Fig 5: Vitiligo associated with alopecia
areata. |
|
 |
Fig 6: Vitiligo associated with psoriasis in
two different cases. |
|
 |
Fig 7: Vitiligo associated with naevus flameous. |
|
 |
Fig 8: Vitiligo associated with squamous cell
carcinoma. |
|
 |
Fig 9: Vitiligo associated with keloid. |
|
Discussion:
Most studies reported that vitiligo affects both sexes nearly equally.[8,9,10,11,12] Some other studies reported a female predominance in their patients. However, in all the above mentioned studies vitiligo was not categorized into types. [13,14] Al Khateeb et al., 2003[15] in his study on NSV patients reported equal affection of both sexes which goes in accordance with our results. Female predominance in our SV patients is in agreement with the study of Barona et al., 1995, [6] but not in agreement with the study of Hann and Lee, 1996. [3] Some authors explained this female predominance by the high cosmetic concern in females.[13,14] We agree with this explanation especially that the disfigurement of the face, the commonest involved site in SV, can not be ignored by females.
Age at onset: Koga and Tango 1988 reported that the onset of NSV could occur at any age whereas SV generally affected the young.[4] In the present study, the mean age at onset in the NSV group was 21.08 years which is in agreement with the studies of Al Khateeb et al., 2003[15] and Barona et al., 1995.[6] Dogra et al., 2005 [7]
analyzed the peak onset of SV in some previous studies [6,12,16,17] and concluded that most cases are acquired early in life between 4 and 12 years. This is in agreement with our results in which the mean age at onset in the SV patients was 8.6 years
Age at presentation: In the present study the mean age at first presentation was 20.07 years in NSV which is lower than that reported by Barona et al., 1995[6] and Al Khateeb et al., 2003.[15] In the SV group, the mean age at presentation was 17.3 years which is in agreement with that reported by Hann and Lee, 1996[3] (20 years) and Barona et al., 1995[6] (19.7years). Other authors did not categorize vitiligo into types.[7,12,14]
Sites of involvement: The predominance of face affection in the SV group in our study is in agreement with the results of Hann and Lee, 1996.[3] In the NSV group, the limbs were the commonest affected site which is in agreement with other studies.[14,15,16,17,18] However in those reports, vitiligo was not categorized as segmental and non- segmental.
Extension of the lesions: In the present study, the majority of the patients in the SV group (84.2%) showed single site affection. This is in agreement with the results of Lerner, 1959 [19] and Hann and Lee, 1996 [3] who reported that 75% and 87% of their SV patients had single lesions respectively. On the other hand in the NSV, lesions are scattered all over the body usually in a symmetrical distribution.[2,16] This goes in accord with our results in which 53.52% of NSV patients showed affection of more than one body site.
Type of vitiligo: Iacovelli et al., 2005 reported that NSV was the most common form of the disease in 83% which is in agreement with our results.[18] SV lesions are reported to be the least frequent type of vitiligo in our patients which is in agreement with other reports.[12,17,20]
Family history: Ninety- nine patients, constituting 9% of the whole study group and 9.67% of the NSV group, reported a positive family history of the disease This result is similar to the findings of Al Khateeb et al., 2003.[15] Onunu and Kubeyinje, 2003,[14] Dogra et al., 2005[7] and Iacovelli et al., 2005[18] reported family history in 18%, 27.3% and 15.9% of their patients respectively. However, these studies did not categorize vitiligo into types. None of the SV patients in our study reported a family history of vitiligo. This is not in agreement with the study of Hann and Lee, 1996[3] who reported positive family history in 11.5% of their SV patients and the study of Barona et al., 1995[6] who found that family history is equally frequent in either types of vitiligo.
Associated medical diseases: El Mofty and El Mofty 1980 [21] and Halder, Nandedkar and Neal, 2003[16] reported that SV is not associated with other autoimmune diseases. Although Koga and Tango 1988 [4] and Barona et al., 1995[6] found that diseases with an autoimmune pathogenesis occurred in their SV patients, yet they reported them more frequently with NSV than in those with SV. In the present study, associated autoimmune diseases were reported in 3.54% of the patients. This figure will be 3.8% and 0% on considering the NSV and SV groups respectively. Other studies, which were not categorizing vitiligo into types, showed contradictive results ranging from 1.3% [22] to 9.5%.[23]
Associated skin Disorders: Lichen planus and vitiligo are common skin disorders, which may rarely coexist.[24] An association between the two may be coincidental.[25] A concomitant immunologic mechanism is one possible explanation for this association.[26] Moreover, PUVA therapy is a well known to give rise to lichenoid changes in vitiliginous skin.[25] However, none of our patients showing this association received PUVA therapy. The association between vitiligo and psoriasis has been known since 1890.[27] Hellgren 1967 found a higher percentage of psoriasis among vitiligo patients than among a normal control population.[28] El- Mofty 1968[29] noted four patients with psoriasis among 545 patients with vitiligo and Boisseau- Garsaud et al., 2000 [11] reported psoriasis in 6% of their vitiligo patients. Handa and Dorga 2003,[22] reported alopecia areata in 0.32% of their 625 vitiligo patients. In the present study, alopecia areata was reported in 12 patients (1.09%). A theoretical explanation for the relationship between alopecia areata and vitiligo had been offered by Lerner 1971.[30] In their study on SV patients, Hann and Lee 1996,[3] reported halo
nevi in 2 patients (0.96%) while Cho et al., 2000 [31] reported halo nevi in 2.5% of children and 4% of adult patients with vitiligo. Our results reported the association of Halo
nevi with NSV in 16 patients (1.45%). Reported cases of skin cancer in chronically light exposed vitiligo patches have been rare. Seo and Kim, 2001[32] reported five cases and Lassus et al., 1972,[33] reported another two cases of vitiligo and skin cancer but it was not specified whether the
tumor occurred in vitiligo lesions or normally pigmented skin. Our study adds another case of squamous cell carcinoma occurring on top of vitiliginous area. Ultraviolet radiation is the major risk factor for the development of cutaneous squamous cell carcinoma. One would expect that the complete absence of melanin pigment in vitiligo increases the deleterious effects of UV light thus increasing the incidence of skin cancer. However, the rareness of reported skin cancer in vitiligo seems to indicate that the absence of melanin doesn't enhance the development of SCC in vitiligo patients.[32] It is worthy to note that all the associated medical and skin diseases in our study were reported in the NSV group only. Conclusion:
In the studied Egyptian group, vitiligo affects both sexes almost equally in the non- segmental vitiligo group while females are predominant in the segmental vitiligo group. The mean ages at onset and at presentation are much earlier in the SV patients. Positive family history and associated diseases are reported only in patients with non- segmental vitiligo only. These findings stress the view considering the segmental and non- segmental vitiligo as two completely different types. Articles dealing with vitiligo either its pathogenesis or therapy should categorise vitiligo into segmental and non- segmental types otherwise, all results will be biased. References
1. Howitz J, Brodthagen H, Schwartz M, Prevalence of vitiligo, Arch Dermatol. 113:47-52,1977.
2. Njoo MD, Westerhof W, Vitiligo: Pathogenesis and treatment, Am J Clin Dermatol. 2:167-181,2001.
3. Hann SK and Lee HJ, Segmental vitiligo: clinical findings in 208 patients, J Am Acad Dermatol. 35(5)671- 674,1996.
4. Koga M, Tango T, Clinical features and course of type A and type B vitiligo, Br J Dermatol. 118:223-228,1988.
5. Koga M. Vitiligo: a new classification and therapy, Br J Dermatol. 97:255- 261,1977.
6. Barona MI, Arrunategui A, Falabella R, Alzate A, An epidemiologic case- control study in a population with vitiligo, J Am Acad Dermatol. 33:621-625,1995.
7. Dogra S, Parsad D, Handa S, Kanwar AJ, Late onset vitiligo: a study of 182 patients, Int J Dermatol. 44:193-196,2005.
8. Mehta NR, Shah KC, Theodore C, Vyas VP, Patel AB, Epidemiological study of vitiligo in Surat area, Indian J Med Res. 61:145-154,1973.
9. Das SK, Majumder PP, Chakraborty R, Majunder TK, Halder B, Studies on vitiligo. I. Epidemiological profile in Calcutta, India, Genet Epidemiol. 2:71-78,1985.
10. Das SK, Majumder PP, Majunder TK, Halder B, Studies on vitiligo. II. Familial aggregation and genetics, Genet Epidemiol. 2:255-262,1985.
11. Boisseau- Garsaud AM, Garsaud P, Cales- Quist D, Helenon R, Queneherve C and Claire RCS, Epidemiology of vitiligo in the French West Indies [Isle of Martinique], Int J Dermatol. 39(1)18-20,2000.
12. Liu JB, Li M, Yang S, Gui JP, Wang HP, Du WH, Zhao, XY, Ren YQ, Zhu YG, Zhang XJ, Clinical profiles of vitiligo in China: an analysis of 3742 patients, Clin Exp Dermatol. 30:327-331,2005.
13. Majunder PP, Nordlund JJ, Nath SK, Pattern of Familial aggregation of vitiligo, Arch Dermatol. 129:994-998,1993.
14. Onunu AN and Kubeyinje EP, Vitiligo in the Nigerian African: a study of 351 patients in Benin City, Nigeria, Int J Dermatol. 42(10)800-802,2003.
15. Al Khateeb A, Fain PR, Thody A, Bennett DC, Spritz RA, Epidemiology of vitiligo and associated autoimmune diseases in Caucasian probands and their families, Pigment Cell Res. 16:208-214,2003.
16. Halder RM, Nandedkar MA and Neal KW, Pigmentary disorders in ethnic skin, Dermatol Clin. 21:617- 628,2003.
17. Zhang XJ, Liu JB, Gui JP, Li m, Xiong QG, Wu HB, Li JX, Yang S, Wang HY, Gao M, Yang J, Yang Q, Characteristics of genetic
epidemiology and genetic models for vitiligo, J Am Acad Dermatol. 51:383-390,2004.
18. Iacovelli P, Singara JLM, Vidolin AP, Marenda S, Capitanio B, Leone G, Picardo M, Prevalence of thyroiditis and of other autoimmune diseases in children with vitiligo, Dermatology. 210:26-30,2005.
19. Lerner AB, Vitiligo, J Invest Dermatol 32:285-310,1959.
20. Handa S, Kaur I, Vitiligo: clinical findings in 1436 patients, J Dermatol. 26(10)653-657,1999.
21. El Mofty AM, El Mofty M, Vitiligo: a symptom complex, Int J Dermatol. 19:238-247,1980.
22. Handa S and Dogra S, Epidemiology of childhood vitiligo: a study of 625 patients from North India, Ped Dermatol. 20(3)207-210,2003.
23. Park KC, Youn JI, Lee YS, Clinical study of 326 cases of vitiligo, Korean J Dermatol. 26:200-205,1988.
24. Tan RSH, Samman PD, Ulcerative colitis, myasthenia gravis, atypical lichen planus, alopecia areata, vitiligo, Proc R Soc Med. 74:195-196, 1974.
25. Porter SR, Scully C and Eveson JW, Coexistence of lichen planus and vitiligo is coincidental, Clin Exp Dermatol. 19:366-367,1994.
26. Anstey A and Marks R, Co-localisation of lichen planus and vitiligo, Br J Dermatol. 128:103-104,1993.
27. Neumann, cited by Margarot J. Le psoriasis in Darier J [ed.]: Nouvelle Pratique Dermatologique, Paris: Masson and Cie. 7: 624, 1936;
28. Hellgren L, Psoriasis, Uppsala, Sweden: Almqvist and Wiksells International Booksellers, p77,1967.
29. El- Mofty AM, Vitiligo and psoralens, New York: Pergamon Press, Inc., p24,1968.
30. Lerner AB, On the aetiology of vitiligo and grey hair, Am J Med. 51: 141,1971.
31. Cho S, Kang HC and Hahm JH, Characteristics of vitiligo in Korean Children, Ped Dermatol. 17(3)189-193,2000.
32. Seo SL and Kim H, Squamous cell carcinoma in a patient with generalized vitiligo, J Am Acad Dermatol. 45(6)S227-229,2001.
33. Lassus A, Apajalahti K, Blomqvist M, Mustakallio M, Kiistala U, Vitiligo and neoplasms, Acta Derm Venereol [Stockholm]. 52:29-32,1972.
© 2006 Egyptian Dermatology Online Journal |









