|
|
Abstract
Dandruff, a clinical condition caused by Malassezia (Pityrosporum) species is of great cosmetic concern all over the world. Dandruff is known to be controlled by fungistatic ingredients in Anti-dandruff shampoos. A comparative study on the efficacy of chemical and herbal anti-dandruff ingredients on 'as is' basis and their performance in market shampoos was done in vitro against Pityrosporum ovale (MTCC 1374). Zinc pyrithione (ZnPTO), ketoconazole and other azole compounds recorded good anti-Pityrosporum activity among the chemical ingredients. Herbal ingredients like tea tree oil, rosemary oil, coleus oil, clove oil, pepper extract, neem extract, and basil extract also recorded anti-pityrosporum activity, but their MIC values are much higher than the synthetic ingredients. Shampoos containing ZnPTO and ketoconazole recorded higher in vitro activities than the shampoos containing herbal AD ingredients. Introduction
Dandruff is a common scalp disorder affecting almost half of the post pubertal population of any ethnicity and both genders. The exact nature and etiology of dandruff has always been controversial since the time of the Greeks, through Sabouraud's era in late nineteenth century till to-date [1]. Dandruff represents 25% of all scalp disorders [2] and is present in an estimated 15-20% of the total population [3] and more than 50% of adult population [4]. The pathogenesis of dandruff involves hyper proliferation, resulting in deregulation of keratinization. The corneocytes clump together, manifesting as large flakes of skin. Essentially keratolytic agents, such as salicylic acid and sulfur, loosen the attachments between the corneocytes and allow them to be washed away with shampooing. Keratolytics soften, dissolve and release the adherent scale seen in dandruff, although the mechanism is not fully understood [5]. The causative agents of dandruff belong to the group of scalp commensal lipophilic yeasts of the genus, Malassezia [6]. Eradicating or controlling the abundance of yeasts appears to be the cleverest strategy for treating dandruff. Using various methods, different clinical and experimental protocols and distinct active ingredients, all indicate that applying antifungal based antidandruff shampoos lead to a stereotyped sequence of events [7]. Several fungistatic compounds have been shown to improve dandruff condition. The main active ingredients include imidazole derivatives such as ketoconazole and other compounds such as selenium sulphide, zinc pyrithione (ZnPTO), piroctone olamine, cipropirox olamine, etc. The ultimate goals of antidandruff products are to remove scales, reduce Malassezia (Pityrosporum) species adherence to corneocytes and inhibit the yeast growth. Besides the chemical substances, there is a wide range of herbal ingredients like pepper extract, basil extract, neem extract, rosemary oil, basil oil, clove oil, coleus oil, tea tree oil which have been documented to have good anti pityrosporum or antidandruff (AD) activity. There are several independent studies on these chemical or herbal substances and their efficacy in AD shampoos. However, there is no comprehensive comparative in vitro study on the AD efficacy of the chemical and herbal substances on 'as is' basis or as a functional ingredient in the formulation (AD shampoo). Hence the present study was undertaken. Materials and Methods
All natural and synthetic ingredients were procured from the local market. P. ovale MTCC 1374 culture was received from IMTECH, Chandigarh, India. The shampoos used in the study were popular brands in the Chennai (India) market, (names not disclosed to avoid any commercial implication). The base shampoo was prepared without any anti-dandruff ingredients.
Minimum Inhibitory Concentration (MIC) [8,9] Twenty four hours broth culture of the test organism was used for the study. Doubling dilution of ingredients were done (5, 2.5, 1.25, 0.6 µg/ml) in the appropriate solvents. The culture (104 cfu/ml) in the Sabouraud Dextrose Broth with olive oil was used for inoculation of the tubes with the test ingredients and incubated at 300 C for 24 hrs. After that, a loop full of broth culture was streaked on a Sabouraud Dextrose Agar (SDA) plate overlaid with olive oil to detect the presence or absence of growth of Malassezia. Agar dilution method was adapted for evaluation of shampoos. Different concentrations viz 2.5, 5, 7.5, 10, 25, 50, 75, 100, 125, 150 mg/ml of shampoos (containing active ingredients) were weighed separately in the petriplates and the molten SDA was poured and mixed thoroughly. Twenty µl of culture was spread over the agar. The plates were incubated at 300 C for 3-5 days. Experiments were done in triplicates with suitable controls.
Zone of Inhibition (ZOI) [10] Twenty- four hours broth culture was swabbed over the surface of Dixon agar. All the active ingredients and the shampoos were dissolved in their respective solvents at 10 mg/ml concentration. A circle of 7 mm diameter was cut at the centre of the agar and 100 µl of the above prepared samples were loaded on the well. Plates were incubated at 30 0 C for 3-5 days. After incubation the zone was measured using zone measuring scale and recorded. Results and Discussion:
The recorded results are presented in Tables 1 & 2, Fig 1 & 2. The lack of ZOI for the oils may be attributed to their inability to diffuse through the agar medium. Among the shampoos, those containing ZnPTO and Ketoconazole recorded higher activity levels. According to our survey in Chennai, India, most of the consumers with dandruff prefer to use shampoos with ZnPTO than any other substances. In the survey conducted in Chennai (Tamil Nadu, India) population (consisting of both sexes) of 324 consumers only 138 were using AD shampoos of which 114 were users of shampoos with ZnPTO (82.6%), 8 were users of shampoo with ketoconazole, 8 were users of herbal shampoos and another 8 were using shampoos with climbazole. A large population (n= 186) were using shampoos with no specific antidandruff ingredients despite having dandruff problem. This could be due to the lack of awareness regarding use of anti-dandruff shampoos or that their dandruff condition may be in the range of mild to moderate which would have been managed by regular hair washing with an ordinary shampoo. The preference to ZnPTO based shampoos by the consumers is mainly because of the better management of dandruff by these shampoos (data not included). The results of the present in vitro studies also justify this stand. ZnPTO besides controlling the proliferation of the causative agent may also heal the scalp by normalizing epithelial keratinization, sebum production, or both [1,5]. Some of the earlier studies have also shown a significant reduction in the numbers of yeast organisms after the application of zinc pyrithione. Ketoconazole is an imidazole derivative, broad spectrum antimycotic agent that is active against Pityrosporum ovale [5] and is effective against many fungi both in vivo and in vitro [11]. It is also effective in many dermatomycoses, including pityriasis versicolor [12]. However, the lower preference to the ketoconazole based shampoos by the consumers may be attributed to the relatively higher costs. However, the people (n=8) who have turned to ketoconazole based shampoos in the present study had extensive dandruff and they have been prescribed to use the shampoos by their dermatologists. Further, even though Metronidazole, Fluconazole have also recorded significant anti-Pityrosporum activity in vitro (MIC and ZOI), their usage (oral/ topical drugs) may be limited to severe manifestations of Malassezia as in conditions like seborrheic dermatitis and pityriasis versicolor. Among the herbal ingredients tea tree oil recorded significant anti-fungal activity. Tea tree oil is the essential oil of the leaves of the Australian Melaleuca alternifolia tree. It is a mixture of hydrocarbons and terpenes, consisting of almost 100 substances. The antimicrobial property is attributed primarily to the major component, terpinen-4-ol. Tea tree oil represents a sound alternative for patients with dandruff who prefer a natural product and who are willing to shampoo their hair daily [5]. In our current study, basil oil and coleus oil recorded the highest activity among the herbal ingredients.
|
Serial No. |
Sample |
MIC |
ZOI (diameter in mm) |
|
Synthetic Ingredients |
|
1. |
Ketoconazole |
2.5 µg/ml |
25 |
|
2. |
Metronidazole |
2.5 µg/ml |
25 |
|
3. |
Fluconazole |
2.5 µg/ml |
25 |
|
4. |
ZnPTO |
5 µg/ml |
25 |
|
5. |
Octopirox |
5 µg/ml |
13 |
|
6. |
Climbazole |
20 µg/ml |
30 |
|
Herbal Ingredients |
|
1. |
Clove oil |
1000 µg/ml |
20 |
|
2. |
Coleus oil |
25 mg/ml |
8 |
|
3. |
Basil oil |
10 mg/ml |
5 |
|
4. |
Tea tree oil |
100 mg/ml |
Nil |
|
5. |
Rosemary oil |
200 mg/ml |
Nil |
|
6. |
Pepper Extract |
80 mg/ml |
Nil |
|
7. |
Neem extract |
100 mg/ml |
Nil |
|
8. |
Basil extract |
100 mg/ml |
Nil |
Table 1: MIC and ZOI for all synthetic and Herbal ingredients
used in commercially available shampoos.
|
Serial No |
Shampoo with Actives |
MIC |
ZOI(diameter in mm) |
|
1 |
Base shampoo |
150 mg/ml |
10 |
|
2 |
1% ketoconazole |
5 mg/ml |
30 |
|
3 |
Shampoo A with 1 % ZnPTO |
5 mg/ml |
27 |
|
4 |
Shmapoo B with 1 % ZnPTO |
5 mg/ml |
27 |
|
5 |
Shampoo C wih 1 % ZnPTO |
5 mg/ml |
27 |
|
|
0.5 % Climbazole |
10 mg/ml |
25 |
|
6 |
0.23 % Climbazole |
25 mg/ml |
23 |
|
7 |
0.15 % Tea tree oil, Rosemary oil |
100 mg/ml |
10 |
Table 2: Anti dandruff activity of commercially available
Shampoos with synthetic and herbal active ingredients.
 | Fig 1:
ZOI for Shampoos with different Active ingredients against P.
ovale 1374 |
|
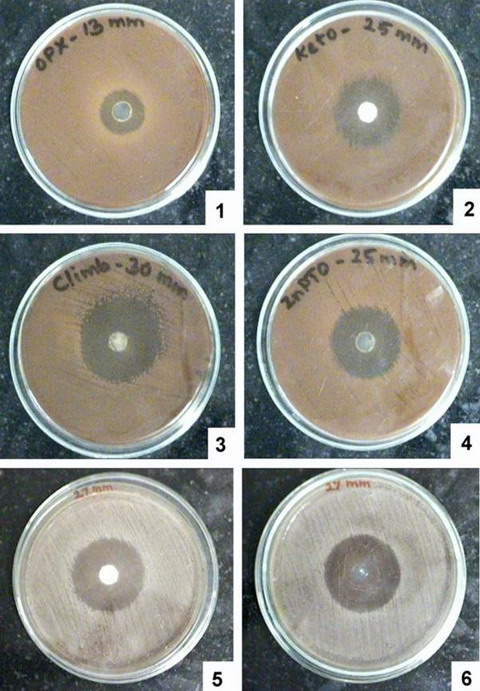 Fig
2: ZOI of different active ingredients against
P. ovale 1374 |
|
Conclusion
This preliminary study showed that Ketoconazole and ZnPTO based shampoos (OTC products) are used more by the consumers for common dandruff problems. The shampoos with ZnPTO are preferred by majority of the consumers not only as the shampoo brands with ZnPTO (AD ingredient) are cheaper but also provide the desired functional benefit. However, in very severe cases of dandruff, ketoconazole based shampoos are preferred despite their relatively higher costs. Herbal ingredients like tea tree oil, rosemary oil, coleus oil, clove oil, pepper extract, neem extract, and basil extract also recorded anti-pityrosporum activity, but their MIC are much higher than the synthetic ingredients. These ingredients can be exploited for its AD activity individually or in combination in AD shampoos. The commercial shampoos with tea tree oil, rosemary oil, henna, lemon also recorded good anti-pityrosporum activity in vitro but not better than shampoos with synthetic ingredients in both MIC and ZOI assays. But for regular usage even shampoos with herbal AD ingredients may suffice the purpose. References
1. Saint-Leger D. The history of dandruff and dandruff in history- A homage to Raymond Sabouraud. Ann Dermatol Venereol. 1990; 117: 23- 27.
2. Herrera-Arellano A, Jimenez-Ferrer E, Vega-Pimentel AM, Martinez-Revera Mde L, Hernandez-Hernandez M, Zamilpa A et al. Clinical and mycological evaluation of therapeutic effectiveness of Solanum chrysotrichum standardized extract on patients with Pityriasis capitis (dandruff): A double blind and randomized clinical trial controlled with ketoconazole. Planta Med. 2004; 70: 483- 488.
3. Selden S, Seborrhoic dermatitis, ed.Travers R, Vinson RP, Meffert J, Quirk C, James WD, eMedicine world library. 2005 Sep 23 [cited 2006 Nov 30]. Available from: URL: http://www.emedicine. com/derm/topic396.htm
4. Ro BI, Dawson TL, The role of sebaceous gland activity and scalp microfloral metabolism in the etiology of seborrhoeic dermatitis and dandruff, J Investig Dermatol Symp Proc. 2005; 10: 194- 197.
5. San Philippo A, English JC. An overview of Medicated shampoos used in Dandruff treatment, P&T. 2006; 31(7): 396- 400
6. Ranjith MS, Gokul Shankar S, Ranganathan S, Sivaramakrishnanan M, Natarajan V, Rasool SK. Role of ABO blood group in the infection rate of dandruff caused by Pityrosporum ovale. Indian J of Dermatol. 2002; 47 (1): 21- 23.
7. Pierard-Franchimont C, Xhauflaire-Uhoda E, Pierard GE. Revisiting Dandruff. International Journal of cosmetic Science. 2006; 28: 311- 318.
8. Krishnamoorthy JR, Ranganathan S, Gokul Shankar S, Ranjith MS, Dano: A herbal solution for Dandruff. African J Biotechnol. 2006; 5(10): 960- 962.
9. Takashi Sugita, Mami Tajima, Tomonobu Ito, Masuyoshi saito, Ryoji Tsuboi, Akemi Nishikawa. Antifungal activites of Tacrolimus and Azole agents against the eleven currently accepted Malassezia sp. J Clin Microbiol. 2005; 2824- 2829.
10. Kumar GS, Jayaveera KN, Ashok kumar CK, Sanjay PU, Vrushabendra Swamy BM, Kishore Kumar DV. Antimicrobial effects of Indian medicinal plants against acne-inducing bacteria. Tropical Journal of Pharmaceutical research. 2007; 6 (2): 717- 723.
11. Heel RC, Brogden RN, Carmin L, Morley PA, Speight TM, Avery GS, Ketoconazole: a review of its therapeutic efficacy in superficial and systemic fungal infections. Drugs 1982; 23: 1- 36.
12. Faergemann, J, Djirv L. Tinea versicolor: treatment and prophylaxis with ketoconazole. Cutis 1982; 30: 542- 550.© 2009 Egyptian Dermatology Online Journal
|


