|
|
Abstract
Nevus comedonicus is a rare adnexal hamartoma of the
pilosebaceous units. Here, a 25 year old Malay fireman with nevus
comedonicus is presented. His nevus comedonicus, comprising of a linear
group of hyperpigmented comedo like papules is seen on the right side of his
neck. There was no associated pain, itching or discharge. He presented
mainly for cosmetic reason. Skin biopsy of the lesion showed the presence
of widely dilated invagination resembling dilated hair follicle filled with
orthekeratotic horny materials penetrating the reticular dermis. The
interfollicular epidermis was normal. Treatment with keratolytics and
topical tretinoin was not satisfactory. He had successful excision of the
lesions.
Introduction
Nevus comedonicus is a rare adnexal hamartoma
involving the pilosebaceous units. It was first reported in 1895 by Kofmann
[1].
Clinically, it presents with linear groups of asymptomatic open comedo-like
pits filled with black keratinous plugs [2,3].
Both unilateral and bilateral distributions are seen [2,4,5].
Face is the most commonly affected site followed by the neck, the trunk and
the upper arms [2].
Here, a case of nevus comedonicus involving the right
side of the neck in a 25 year old Malay man from Miri, Sarawak is reported.
Case report
A 25 year old man presented with multiple papular
lesions on the right side of the neck since childhood. He presented to the
skin clinic because he was embarrassed of the lesions. He was always teased
by fellow colleagues in the fire and rescue department where he works. The
lesions were not painful or itchy. There was no discharge. No other family
members had similar skin lesions.
On examination, there were linear, grouped, hyperpigmented, comedo like,
keratotic papules on the right side of his neck in an area measuring 4 cm X 3 cm (Figure 1). There were no
other lesions on his body
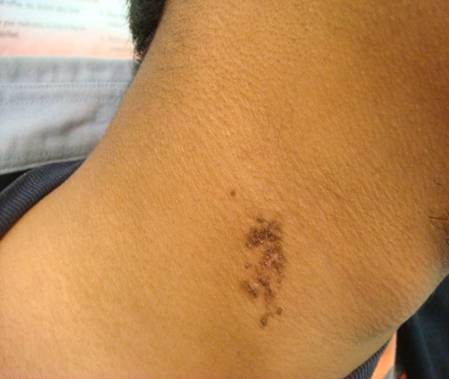 |
Fig 1:
Linear group of comedo-like hyperpigmented papules on the right side
of the neck. |
|
Skin biopsy of one of the comedo like papule showed
deep and wide invagination resembling dilated hair follicle lined by
epithelium and filled with orthekeratotic horny materials penetrating the
reticular dermis (Figure 2, 3). The interfollicular epidermis was
normal. This finding was consistent with the diagnosis of nevus sebaceous.
 |
Fig 2:
Presence of widely dilated invagination resembling dilated hair
follicle filled with orthokeratotic keratinous plug with
perifollicular hyperkeratosis, acanthosis and papillomatosis.
Hematoxylin and eosin. Magnification X 4. |
|
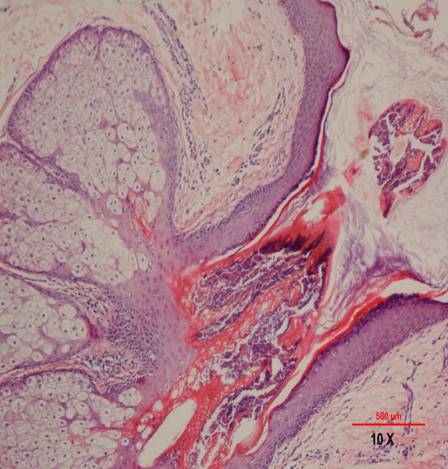 |
Fig 3:
Close up view of the orthokeratosis. |
|
He was given topical 20%
salicylic acid ointment and topical tretinoin
locally
for the lesions. On follow up 2 months later, no satisfactory regression was
seen. He had successful excision of the lesions.
Discussion
Nevus comedonicus is an uncommon developmental anomaly
also known as nevus acneiformis, zoniform nevus with comedones and
systematized sebaceous gland nevus [4].
It is reported in all racial groups. It affects both sexes equally. It could
be present at birth but is usually seen in childhood. Most patients present
before the age of 10 [6].
Familial cases of nevus comedonicus are seen with variable mode of
inheritance [7].
The etiology of nevus comedonicus is unknown. Some
consider it as a hamartoma arising from a defective mesoderm, while others
consider it to be an epidermal nevus involving the appendages namely the
hair follicle and the sweat ducts [8,9,10].
Proponents of defective mesodermal theory postulated that there is
developmental failure of the mesodermal pilosebaceous complex resulting in
imperfect differentiation of the epidermal component. The follicular
structure that forms is unable to generate hair matrix cells. Nevertheless,
it is able to produce the soft keratin that plugs the adnexal orifice,
forming the comedones [2,11].
Those favoring the epidermal nevus theory found epidermolytic
hyperkeratosis, acanthosis and papillomatosis in histopathology, findings
that are characteristically seen in epidermal nevus [12].
Clinically, nevus comedonicus can present in 2
clinical entities. The first is the asymptomatic comedo like eruptions and
the second is the presence of cysts, scars, fistulas, and abscesses due to
inflammation and infection of the comedo like lesions [3,13].
The comedo like eruptions consist of asymptomatic, grouped, usually 20 to 50
small, pin head, hyperpigmented papular lesions. Small comedones appear as
keratin filled pits while larger ones extend above the surface of
surrounding skin and give a `nutmeg crater' feeling. The keratin material
can be shelled out freely, leaving craters in the normal skin. These lesions
are usually seen on the face, neck, trunk and upper arm. Albeit rare, there
are also reported on the palms, scalp, ears and genitalia [14,15,16,17].
The lesions can cover an area as small as 2 cm to extensive involvement of
the body [2,4,5,18,19].
Most of the lesions are unilateral and segmental, following the lines of
Blascko [4].
Approximately 50% of patients with nevus comedonicus
will present with the second clinical entity. The recurrent inflammation and
infection in this entity poses a more severe clinical problem for both the
patients and the treating physician as it will lead to abscesses, cysts,
fistulas and eventually scars; as opposed to the mainly cosmetic problem
poses by the first entity. This entity is more commonly seen in adolescents
and adults as the inflammatory disease activity and severity increases with
age [3].
Follicular tumors have been reported to occur within
the nevus comedonicus. These tumors include trichofolliculoma and pilar
sheath acanthoma [20,21].
Epidermoid cyst, trichilemmal cysts, linear cell nevus, ichthyosis and
Alagille syndrome have also been associated with this condition [22,23,24,25,26].
Association with extracutaneous manifestations especially neurological,
ocular and skeletal anomalies have been termed nevus comedonicus syndrome [5,27].
These anomalies include electroencephalographic abnormalities, ipsilateral
cataract, corneal changes, hemivertebrae, scoliosis and absence of the fifth
ray of a hand [28].
Histopathological examination shows large dilated
pilosebaceous follicles filled with orthokeratotic keratin materials [4,13].
One to several hair shafts can be found occasionally on the base of the
lesion. Similarly, small sebaceous gland lobules may be seen opening into
the lower pole of the invaginations [4].
The interfollicular epidermis shows hyperkeratosis and papillomatosis
resembling epidermal nevus. Occasionally, epidermolytic hyperkeratosis is
seen [12].
Inflamed and infected lesions will show presence of dermal inflammatory
cells infiltrates.
Nevus comedonicus needs to be differentiated from
linear epidermal nevus, comedonal acne, lymphangioma and lichen striatus
clinically. The differential diagnosis for the inflamed entity includes
inflammatory linear verrucous epidermal nevus and its variants; linear
lichen planus and linear psoriasis. Differentiation of nevus comedonicus
with other epidermal nevi is easy as the former shows presence of comedones,
which on extraction will leave a crater on the skin surface. Finding groups
of lesions following the lines of Blascko excludes comedonal acne.
Lymphangioma circumscriptum usually presents as groups of vesicle like
papules resembling frog spawns, unlike the comedonal lesions of nevus
comedonicus. Histologically, differentiation from comedonal acne is
important. In comedonal acne, the pilosebaceous units are complete whereas
those in nevus comedonicus are poorly formed. Moreover, in nevus
comedonicus, hyperkeratosis and papillomatosis are frequently observed in
the interpapillary epidermis and absent in comedonal acne. Dilated pore of
Winer can sometimes be confused with nevus comedonicus histologically.
However, this condition is usually seen in the elderly and can be
differentiated clinically.
Treatment of nevus comedonicus is mainly for cosmetic
reason. However, for those with the inflamed entity, proper treatment is
needed to prevent complications of the recurrent infection and inflammation.
Various types of treatment have been used to treat nevus comedonicus.
Treatment outcomes are mostly unsatisfactory [4,15].Topical
agents like tretinoin, ammonium lactate lotion, tazarotene and calcipotriol
have been reported to be cosmetically successful by some [29,30,31].
Pore strips to eliminate keratin plugs have also produced excellent cosmetic
outcome in a Japanese patients [13].
Erbium-YAG laser have also been reported to be successful [32].
Dermabrasion, carbon dioxide lasers and comedo extraction have all been used
with variable success [33].
Topical and systemic antibiotics are usually needed in the inflamed entity.
Use of oral isotretinoin may partially suppress the inflammation but many
fail to respond [34].
The comedonal lesions do not respond to oral isotretinoin. Surgical excision
is useful especially in limited areas of inflammation [34].
In conclusion, nevus comedonicus is a rare
developmental anomaly causing mainly cosmetic disfigurement. Complications
due to recurrent inflammation and infection can occur. Treatment outcome
both cosmetically and medically are variable. A classical case of nevus
comedonicus with poor topical treatment outcome but successful surgical
excision was presented.
References
1. Kofmann S. Ein fall Von Seltener Lokalisation and Verbreitung Von Komedonen, Arch Derm Syphilol 1895; 32: 177- 178.
2. Sharma RP, Singh SP. Extensive unilateral nevus comedonicus with bilateral involvement of face. Indian J Dermatol Venereol Leprol 2001; 67: 195- 6. PMID: 17664739.
3. Vasiloudes PE, Morelli JG, Weston WL. Inflammatory nevus comedonicus in children. J Am Acad Dermatol 1998; 38: 834- 6. PMID: 9591797
4. Gharpuray BM, Mutalik S. Nevus unilateralis comedonicus. Indian J Dermatol Venereol Leprol 1990; 56: 448- 9.
5. Alpsoy E, Durusoy C, Ozbilim G, Karpuzoglu G, Yilmaz E. Nevus comedonicus syndrome: a case associated with multiple basal cell carcinomas and a rudimentary toe. Int J Dermatol 2005; 44(6): 499- 501. PMID: 15941441.
6. Beerman HB, Van Meter RH. Nevus comedonicus. Arch Derm Syphilol 1949; 60(1): 130. PMID: 18229377.
7. Giam YC, Ong BH, Rajan VS. Nevus comedonicus in homozygous twins. Dermatologica 1981; 162(4): 249- 53. PMID: 7196349.
8. Lefkowitz A, Schwartz RA, Lambert WC. Nevus comedonicus. Dermatology 1999; 199(3): 204- 7. PMID: 10592398.
9. Kim SC, Kang WH. Nevus comedonicus associated with epidermal nevus. J Am Acad Dermatol 1989; 2: 1085- 8. PMID: 2808839.
10. Nabai H, Mehregan AH. Nevus comedonicus. A review of literature and report of twelve cases. Acta Dermatol Venereol; 1973; 53(1): 71- 4. PMID: 4120812.
11. Wood MG, Thew MA. Nevus comedonicus: a case with palmar involvement and review of literature. Arch Dermatol 1968; 98(2): 111- 6. PMID: 5667222.
12. Morillo V, Manrique P, De Miguel E, Arechalde A, Mariscal A. Nevus comedonicus with epidermolytic hyperkeratosis.Eur J Dermatol. 2007; 17(2): 176- 7. PMID: 17337416.
13. Inoue Y, Miyamoto Y, Ono T. Two cases of nevus comedonicus: Successful treatment of keratin plugs with a pore strip. J Am Acad Dermatol 2000; 43: 927- 9. PMID: 11044825.
14. Riyaz N, Riyaz A. Nevus comedonicus affecting the palms. Indian J Dermatol Venereol Leprol 1998; 64: 197- 8.
15. Ghorpade A, Ramanan C. Penile nevus comedonicus. Indian J Dermatol Venereol Leprol 1991; 57: 237- 9.
16. Harper KE, Spielovogel RL. Nevus comedonicus of the palm and wrist. Case report with review of five previously reported cases. J Am Acad. Dermatol 1985; 12: 185- 8. PMID: 3973117.
17. Asokan N, Sridevi PK. Inflammatory nevus comedonicus in an infant. Indian J Dermatol Venereol Leprol 2008; 74(6): 658- 9. PMID: 19172001.
18. Fletcher CL, Acland KM, Powles AV. Unusual giant comedo nevus. Clin Exp Dermatol 1999 May; 24(3): 186- 8. PMID: 10354176.
19. Beck MH, Dave VK. Extensive nevus comedonicus. Arch Dermatol 1980; 116(9): 1048- 50.PMID: 7416758.
20. Dudley K, Barr WG, Armin A, Massa MC. Nevus comedonicus in association with widespread, well-differentiated follicular tumors. J Am Acad Dermatol 1986; 15: 1123- 7. PMID: 3771864.
21. Lee HJ, Chun EY, Kim YC, Lee MG. Nevus comedonicus with hidradenoma papilliferum and syringocystadenoma papilliferum in the female genital area. Int J Dermatol. 2002 Dec; 41(12): 933- 6. PMID: 12530358.
22. Mathur KD, Bhargava P, Agarwal US, Math. Nevus comedonicus associated with epidermoid cyst. Indian J Dermatol Venereol Leprol 1996; 62: 250- 1.
23. Carney RG. Linear unilateral basal cell nevus with comedones: report of a case. AMA Arch Derm Syphilol 1952; 65(4): 471- 6. PMID: 14902117.
24. Leppard BJ. Trichilemmal cysts arising in an extensive comedo nevus. Br J Dermatol 1977; 96(5): 545- 8. PMID: 871391.
25. Piers F. Linear comedo nevus and ichthyosis. Br J Dermatol 1945; 57: 138- 47.
26. Woods KA, Larcher VF, Harper JI. Extensive nevus comedonicus in a child with Alagille syndrome. Clin Exp Dermatol 1994; 19(2): 163- 4. PMID: 8050150.
27. Engber PB: The nevus comedonicus syndrome: A case report with emphasis on associated internal manifestations. Int J Dermatol 1978; 17(9): 745- 749. PMID: 730460.
28. Sugarman JL. Epidermal nevus syndromes. Semin Cutan Med Surg 2007; 26(4): 221- 230. PMID: 18395670.
29. Blanchard L, Hodge SJ, Owen LG. Linear eccrine nevus with comedones. Arch Dermatol 1981; 117(6): 357- 9. PMID: 7247428.
30. Milton GP, DiGiovanna JJ, Peck GL. Treatment of nevus comedonicus with ammonium lactate lotion. J Am Acad Dermatol 1989; 20: 324- 8. PMID: 2915076.
31. Deliduka SB, Kwong PC. Treatment of nevus comedonicus with topical tazarotene and calcipotriene. J Drugs Dermatol 2004; 3(6): 674- 6. PMID: 15624751.
32. Caers SJ, Van der Geer S, Beverdam EG, Krekels GA, Ostertag JU. Successful treatment of nevus comedonicus with the use of the Erbium Yag laser.J Eur Acad Dermatol Venereol. 2008; 22(3): 375- 7. PMID: 18005024.
33. Loria PR, Hailey CW. Nevus follicularis keratosis (comedo nevus): review of world literature and addition of a case. Arch Dermatol 1961; 83: 991- 4. PMID: 13763543.
34. Milburn S, Whallett E, Hancock K, Munnoch DA, Stevenson JH. The treatment of nevus comedonicus. Br J Plast Surg 2004; 57(8): 805- 6. PMID: 15544785.
© 2009 Egyptian Dermatology Online Journal |



