Summary
Cutaneous vasculitis is a rare complication of rifampicin therapy. Herein we describe a case of a vasculitis of the skin induced by rifampicin in the course of an anti tuberculosis therapy. The patho-physiological mechanism is likely to be the presence of anti-rifampicin antibodies responsible for the formation of immune complexes. Differential diagnoses include vasculitis induced by other associated drug therapy, particularly anti tuberculosis ones and vasculitis related to the infectious process, itself, including tuberculosis.
Introduction
Rifampicin is widely used in the treatment of tuberculosis and may be given either daily or intermittently [1]. This drug has been associated with a variety of adverse effects. A relatively uncommon side effect is cutaneous vasculitis. We report cutaneous vasculitis in association with therapy with rifampicin. A few cases have been reported to our knowledge.
Case Report: A 45- year-old woman was admitted for tuberculosis mono-arthritis of the right knee. Standard quadruple anti-tuberculosis chemotherapy was begun with rifampicin (600 mg/d), isoniazid (400 mg/d), streptomycin (500 mg/d) and ethambutol (800mg) was instituted. Fifty days after initiation of treatment, she developed a maculopapular rash on the abdomen, the upper limbs and principally on the lower limbs (Fig 1). In addition, physical examination revealed the patient to be in a good general health. Urinalysis showed no blood or protein and renal function test was normal.
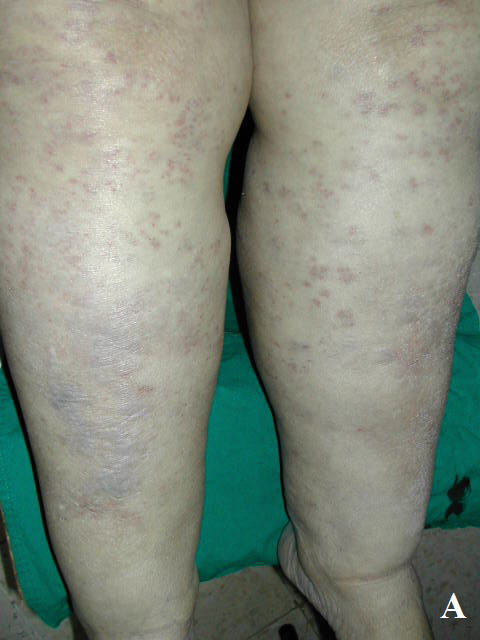
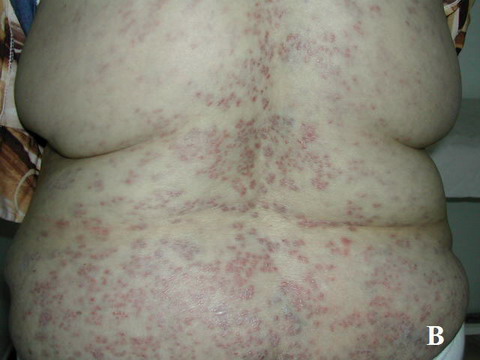
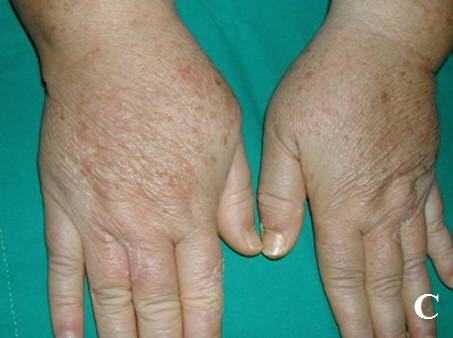 | Fig 1:
Extensive and infiltrated purpura on lower limbs (A), trunk (B) and
upper limbs (C). |
|
Laboratory analysis showed negative antinuclear antibody and rheumatoid factor, the complement was normal. The haemoglobin level and platelets counts were normal. A skin lesion biopsy revealed cutaneous leucocytoclastic vasculitis. Stopping the streptomycin therapy did not affect the rash; however when rifampicin was stopped, the patient showed improvement and the purpura gradually disappeared. Rifampicin was the drug incriminated. Our patient was then treated by three drugs, which ware isoniazid, ethambutol and pyrazinamid with no recurrence of the purpuric rash on the skin. The patient was discharged from the hospital after a few days.
Discussion
Adverse effects of antituberculosis chemotherapy are well recognized [2]. Ethambutol can produce purpura, streptomycin can cause a polyarteritis-like syndrome and isoniazid can cause a lupoid reaction [2]. However, cutaneous vasculitic associated with rifampicin therapy has only few reports [3]. Drugs induced vasculitis usually develops within seven to 21 days after a drug is started and may be confined to the skin [4,5]. Skin lesions are identical to those seen in systemic small vessel vasculitis [5]. In our case, a maculopapular rash appeared fifty days after the initiation of anti-tuberculosis chemotherapy. Cutaneous vasculitis associated with tuberculosis may occur by [3,6,7]: a- direct invasion of the vessel wall by tubercle bacilli b- immunological reaction involving the deposition of immune complexes c- intra-vascular release of mycobacteria followed by Arthus reaction and delayed hypersensitivity response or d- rifampicin-dependent antibody and immune complex formation. In cases of tuberculosis-related vasculitis, the skin lesions improve with introduction of the treatment regimen, without the need for specific anti-inflammatory treatment [6]. In vasculitis caused by medications (such as rifampicin), it is recommended that the medication be discontinued and replaced by an alternative regimen, that results in clear lesion improvement [7]. Anti-histamines and non steroidal anti-inflammatory drugs can be used for symptomatic treatment [7]. Severe skin manifestations can be treated with corticosteroids, the use of which was not necessary in our patient [4]. The cutaneous vasculitis of our case was probably related to rifampicin, the diagnosis was suggested by the disappearance of symptoms after rifampicin withdrawal although the immune complexes and rifampicin antibody levels were not measured in our patient. Thrombocytopenic purpura was excluded by the normal platelet count in this case.
Conclusion
Cutaneous vasculitis associated with rifampicin therapy is rare. A few cases have been reported to our knowledge. As this drug is widely used such reactions are therefore important to note. References
1. Cohn J, Fye D, Sills J, Francos G. Rifampicin -induced Renal Failure. Tubercle 1985; 289- 293.
2. Iredale J, Sankaran R, Wathen C. Cutaneous vasculitis associated with rifampicin therapy. Chest 1989; 96(1): 215- 216.
3. Chan S, Chong Y, Sun A, Hoheisel G. Cutaneous vasculitis associated with tuberculosis and its treatment. Tubercle 1990; 71: 297- 300.
4. Jennette C, Ronald J. Small-vessel vasculitis. The New England Journal of Medicine 1997; 337 (21): 1512- 1523.
5. Narang S, Khan A, Gupta A. c-ANCA Vasculitis with Tubercular Osteomyelitis. JIACM 2007; 8(2): 182- 184.
6. Hee M, Yong P, Ho Y, Soo L. Cutaneous leukocytoclastic vasculitis with cervical tuberculous lymhadenitis: a case report and literature review. Rheumatol Int 2006; 26: 1154- 1157.
7. Carvalho M, Dominoni R, Senchechen D, Fernandes A, Burigo I, Doubrawa E. Cutaneous Leukocytoclastic vasculitis accompanied by pulmonary tuberculosis. J Bras Pneumol 2008; 34(9): 745- 748.© 2010 Egyptian Dermatology Online Journal | 


