|
|
Abstract
Inguinal hernia surgery and repair is one of the most commonly
performed surgeries worldwide. The use of mesh has been an advance in
hernia surgery. Complications such as infection, contraction, rejection
of the mesh are known to occur following the repair. We report a case of
a patient who underwent inguinal hernia surgery with mesh repair,
thereafter she developed a sinus opening into the external genitalia in
the late post operative period and presented to us as a case of genital
ulcer.
Introduction
The use of meshes in hernia repair has become common. However, it may
be associated with infectious and non- infectious complications. The
reported incidence of mesh related infections, have been up to 8%. Rate
is influenced by underlying co-morbidity and immuno-suppression [1].
We report one such patient, who developed secondary infection of the
mesh used in the hernioplasty and presented to us with a genital ulcer.
Case History
A 48 year old, married, multiparous female, on treatment for diabetes
and hypertension since the past 10 years had left inguinal hernia since
the past 20 years and right inguinal hernia since 5 yrs. She had an
episode of strangulation of the right hernia sac and had to undergo
emergency bilateral hernioplasty with mesh repair. After 2 months of
uneventful post operative period, she developed lower pelvic pain. Five
months later she noticed a swelling over the right labia majora and the
adjacent area of the mons pubis which progressively increased in size
and 2 months later started discharging mucopurulent discharge via an
opening on the right labia majus.
She also had low grade fever on and off since 3 months. There was no
history of chronic cough, weight loss, noticing any lump in the abdomen,
or exposure to Kochs patient. There were no history of extramarital
sexual exposure, no vaginal discharge or ulcer in the past and no
abortion or use of contraceptive devices.
Examination revealed a conscious, oriented female with stable vitals.
There was no pallor, icterus, cyanosis or clubbing. Locally, in the
genital region, there was a boggy swelling extending from the right
labia majus to the corresponding area of the mons pubis. The swelling
was erythematous, warm and tender, surface of which showed an ulcer
covered with thick, yellowish, non foul smelling mucopurulent discharge
(Fig. 1). Clearing of the discharge revealed an underlying oval ulcer
measuring approximately 0.6 x 0.4cm. The margin was well defined; the
edge was sloping at places while at other places it was edematous. The
floor was covered with slough. The surrounding skin was erythematous and
edematous. On palpation the ulcer was tender but did not bleed on touch.
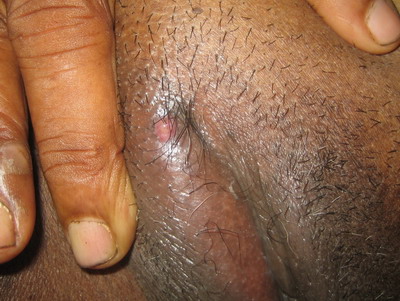 | Fig 1:
Image of the ulcer on the right labia majora. |
|
Bilateral inguinal lymph nodes; the medial group of horizontal chain
as well as the vertical chain were enlarged, the largest being 3x3 cm in
size. All the nodes were discrete, firm, mobile and non tender.
Abdominal examination showed bilateral linear scars present in the
inguinal region, suggestive of previous hernioplasty; however on
palpation there was no tenderness, guarding, rigidity or any
organomegaly noted.
Central nervous system, respiratory system and cardiovascular system
appeared to be unaffected. The rest of the skin and oral mucosa appeared
normal.
Her baseline investigations showed a raised total count which was 13,
600 cells/cm3 with neutrophilia, N80 L15 E5. Her Fasting blood sugar (FBSL)
was 194 mg/dl and Post prandial blood sugar ( PPBSL) was 203 mg/dl. Pus
for gram stain revealed gram positive cocci in clusters. Pus culture and
sensitivity showed growth of staphylococcus aureus, sensitive to
linezolid. Smear for Acid Fast Bacilli detection, as well as Potassium
hydroxide (KOH) for fungal demonstration proved negative. Tests for
syphilis such as VDRL test and Treponema Pallidum Hemagglutination (TPHA)
test were both negative, as also the tuberculin test for tuberculosis
and ELISA test for HIV infection were negative. Based on the initial
presentation, a tentative diagnosis of genital ulcer disease (GUD) was
made and she was treated for the same, based on syndromic approach as
per NACO guidelines [2]. However, the
ulcer remained unchanged. Thereafter, based on pus culture and
sensitivity, which had arrived by then, she was started on oral
linezolid, which she received for 2 weeks. Unfortunately, the ulcer did
not respond. The non healing behaviour of the ulcer as well as the
periodic discharge from it led us to suspect a presence of sinus in her.
Hence, abdominal Ultrasonography (USG) and a Sinogram were done. USG
revealed a well defined hypodense collection in the anterior pelvic wall
on the right side. The Sinogram showed the dye outlining the sinus
tract, extending from the cutaneous opening and going up to the origin
of the sinus. This origin was seen to be situated laterally at the level
of the right superior pubic rami with collection of the dye in the
adjacent anterior abdominal wall. There was no contrast leak into the
peritoneal cavity. With the above findings, the presence of a sinus was
confirmed. Opinion taken from the surgeon stated that the sinus probably
was secondary to the infected mesh and the appropriate approach was to
re-explore and remove the infected mesh. However the patient was lost
for follow up.
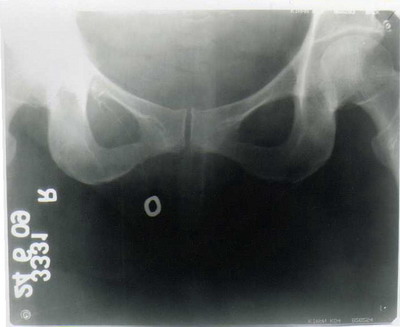 | Fig
2: Sinogram showing collection of the dye at the level of
Right pubic ramus. |
|
Discussion
We present a case of a female patient who presented to us with a
genital ulcer. Failure to respond to all the treatments given led us to
suspect a sinus in her for which she was evaluated. Sinogram confirmed
the presence of a sinus. This was in fact the site of the infected mesh
used in the hernioplasty procedure. However, tuberculosis as a cause of
chronic ulcer was ruled out, there being no significant positive history
as also chest X-ray, PPD and AFB staining were negative.
The patient's uncontrolled diabetic profile could have been a
confounding factor. Thus, the infection progressed, finally following
the path of least resistance, and presented as a genital ulcer, which
actually was the opening for a chronic draining sinus.
The primary benefit of using a mesh is to reduce recurrence. Mesh
materials available range from absorbable to non absorbable and from
inert to biologic [3].Serious
complications have been observed in a small percentage of patients,
these include wound infection with or without chronic draining sinuses,
erosion into adjacent structures including the intestine, extrusion of
the material, entero-cutaneous fistula, small bowel obstruction and
recurrent herniation.[4]
Prophylactic antibiotic usage is important. Inspite of that, Houck et
al [5] and White et al [6]
have reported an infection rate of 15% and 14% respectively. Molloy et
al reported a sinus formation rate of 12% [7].
Propylene mesh was associated with significantly greater chronic
inflammatory reaction and fibrosis [8].
In our patient, so also, a polypropylene mesh was used.
Sores mistaken to be sexually transmitted, infective in origin have
been reported by V.L.Rege and P.Shukla, 1993(9). Similarly, VS
Hanchanale et al., 2006 reported a patient presenting with gluteal
sinus, which was later diagnosed to be due to renal tuberculosis [10].
In both the above cases, a Sinogram was used to confirm the diagnosis of
the presence of a sinus tract.
References
1. Bliziotis A, Kasiakou SK, Kapaskelis AM and Falagas
ME. Mesh-related infections after hernia repair: Case Report of an
Emerging type of Foreign body related infection. Infection.Vol 34,
number 1 /February 2006, Pages 46-48
2.
www.nacoonline.org
3. Robinson TN, Clarke JH, Schoen J, Walsh MD. Major
mesh-related complications following hernia repair. Surg Endosc 2005;
19: 1556- 1560
4. Basoglv M, Yildirgan MI, Yilmar I, Balik A, Celebi F,
Atamanalp SS, Polat KY, OrenD. Late complications of Incisional Hernias
following prosthetic mesh repair. Acta Chir Belg 2004; 104: 425- 428
5. Houck J P, Rypins E B, Sarfeh I J, Juler G L, Shimoda
K J Repair of Incisional Hernia. Surg Gynecol Obstet 1989; 169: 397- 399
6. White T J, Santos M C, Thompson J S Factors affecting
wound complications and repair of ventral hernias. Am Surg1998; 64: 276-
280
7. Molloy R G, Moran K T, Waldron R P, Brady M P and
Kirwan W O. Massive incisional hernia : abdominal wall replacement with
marlex mesh Br J Surg 1991; 78: 242- 244
8. Stockheld DG, Granstrom L, Backman L, Dahlgren S.
inflammatory response to subcutaneously implanted marlex and Gore-tex in
massively obese patients, Biomaterials 1992; 13: 261- 263
9. Rege VL, Shukla P. Osteomyelitis presenting as a
genital sore - a case report. Genitourin Med 1993; 69: 460- 461
10. Hanchanale VS, Rao AR, Motiwala HG. Renogluteal
Fistula - An unusual complication of genitourinary tuberculosis. IJDVL
2006; 22(3): 270- 271.© 2011 Egyptian
Dermatology Online Journal
|


