|
|
Abstract
Bullous pemphigoid is typically a disease of the elderly, with an onset
after 60 years of age. It is the most common autoimmune subepidermal blistering
disease of the skin which presents with generalized pruritic bullous eruption.
The spectrum of clinical presentation is extremely broad and rare clinical
variants have been reported in literature. We describe a patient who presented
with ulceration of the nose of 3 months duration. He denied history of vesicles,
bullae or urticarial lesions. The clinical diagnosis of granulomatous inflammation
was considered. Biopsy done from the nose and buccal mucosa showed subepithelial
eosinophil and neutrophil rich bullous lesion suggestive of bullous pemphigoid.
On immuno-histochemistry, the floor of the bulla showed positive staining
for laminin. The patient later developed tense vesicles and bullae over
the trunk and thighs. He showed complete resolution of the skin lesions
within a week of starting oral steroid therapy. These findings suggest our
patient had an atypical, non-bullous presentation of the pemphigoid spectrum.
Introduction
Bullous pemphigoid (BP) is the most common autoimmune blistering disorder
occurring in the elderly population presenting with tense erythematous blisters
occurring on healthy or normal skin.[1] It is usually a
chronic disease, with spontaneous exacerbations and remissions, which may
be accompanied by significant morbidity. The presentation of BP is polymorphic
and initially misdiagnosed and in early or atypical cases, full- blown bullous
lesions may be completely absent. In these cases, establishing the diagnosis
of BP requires a high degree of suspicion and it is important for prompt
institution of appropriate treatment.
We report an unusual presentation of BP which clinically resembled a
granulomatous inflammation. The diagnosis of BP was made on the basis of
skin biopsy.
Case report
A 65 year old gentleman presented with an asymptomatic, gradually progressive
ulcer over the tip of the nose of 3 months duration. He denied the appearance
of vesicles, bullae or urticarial lesions and also denied trauma to the
site of the lesion. There was no history of travel outside his state and
he was treated for pulmonary tuberculosis 15 years ago. There was no history
of photosensitivity, joint pains or oral ulcers and he did not have any
systemic complaints.
Examination revealed an infiltrated, crusted, plaque with erythematous
margins over the tip of the nose (Fig 1). Mucosal infiltrations were
noted on the buccal mucosae (Fig 2). Palms and soles were spared
and rest of the cutaneous and systemic examination was normal. A clinical
diagnosis of granulomatous inflammation was made.
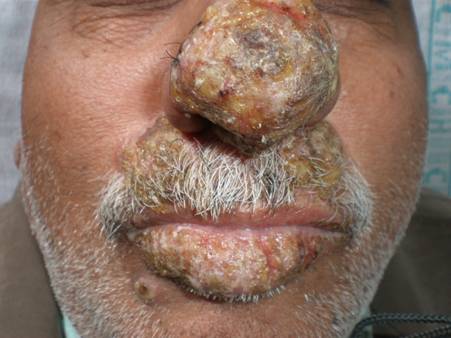 | Fig 1:
Well defined crusted plaques over the nose, lips and moustache
area. |
|
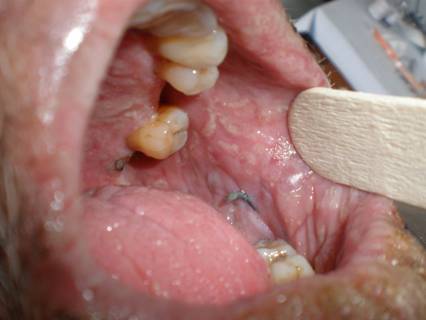 | Fig
2: Mucosal infiltration over the hard palate and buccal
mucosa. |
|
Tissue cultures from the site did not grow fungal or bacterial elements.
Biopsy done from the nose and buccal mucosa showed subepithelial eosinophil
and neutrophil rich bullous lesion with spongiosis and occasional necrotic
keratinocytes (Fig 3). On immuno-histochemistry, the floor of the
bulla showed positive staining for laminin. Immuno-histochemistry for collagen
4 was non-contributory. A possibility of bullous pemphigoid was considered.
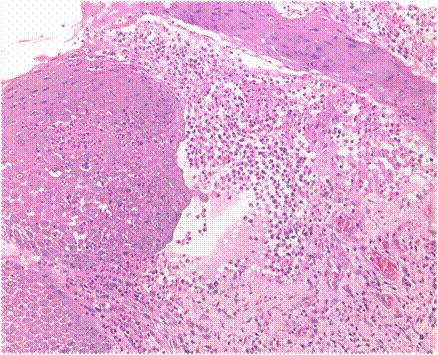 | Fig
3: On H & E stained section (40X): Subepithelial eosinophil
and neutrophil rich bullous lesion with spongiosis and
occasional necrotic keratinocytes. |
|
This patient re-presented after 2 weeks with new lesions on the lips
and chin. Examination revealed yellowish crusted erosions over the lips
and moustache area. A single yellowish plaque studded with pustules was
present on the right mandibular area. A week later he developed tense vesicles
and bullae over the groins and axillae. Since the histopathological diagnosis
was established, repeat skin biopsy or direct immunoflorescence study from
the new lesions was not done.
Patient started oral steroids at 1mg/kg/day and resolution of the cutaneous
and mucosal lesions was noted within a week of initiation of therapy
(Fig 4).
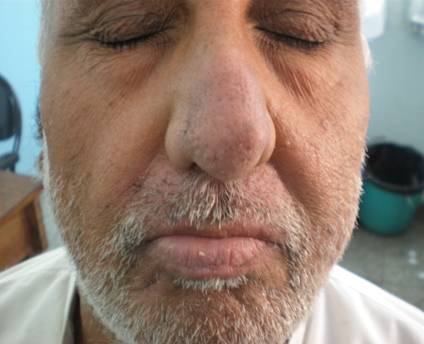 | Fig
4: One week after treatment with oral steroids. |
|
Discussion
Bullous pemphigoid, when presenting with tense pruritic blisters developing
on either healthy or erythematous skin, is easily recognized. There may
be mucosal involvement with blisters and erosions.[2] It
is twice more common in males.[3]
The clinical hallmark of BP is the presence of widespread tense bullae,
which may arise from normal (non-inflamed bullae) or erythematous (inflammatory
bullae). They can occur anywhere, but there is a predilection for the groin,
lower abdomen and the flexural surface of limbs.[2]
Rarely, non bullous manifestations of BP such as non bullous form, those
presenting with exfoliative erythroderma, dyshydrotic eczema, prurigo nodularis,
subacute simple prurigo, ecthyma gangrenosum are documented in literature.[4,5,6,7,8]
Our patient's presentation was a diagnostic challenge due to the lack
of the characteristic morphologic features of BP, namely vesicles or bullae
at the time of presentation. It re emphasizes the need for diagnostic biopsies
and immuno-histochemistry in elderly patients with atypical presentations.
These patients should be followed up regularly as they are at risk for developing
a generalized eruption later in life.
References
1. Kirtschig G, Wojnarowska F. Autoimmune blistering diseases:
an up-date of diagnostic methods and investigations. Clin Exp Dermatol.
1994 Mar;19(2): 97- 112.
2. Korman NJ. Bullous pemphigoid. The latest in diagnosis,
prognosis, and therapy. Arch Dermatol. 1998 Sep;134(9): 1137- 1141.
3. Jung M, Kippes W, Messer G, Zillikens D, Rzany B. Increased
risk of bullous pemphigoid in male and very old patients: A population-based
study on incidence. J Am Acad Dermatol. 1999 Aug; 41(2 Pt 1): 266- 268.
4. Strohal R, Rappersberger K, Pehamberger H, Wolff K. Nonbullous
pemphigoid: prodrome of bullous pemphigoid or a distinct pemphigoid variant?
J Am Acad Dermatol. 1993 Aug; 29(2 Pt 2): 293- 299.
5. Alonso-Llamazares J, Dietrich SM, Gibson LE. Bullous
pemphigoid presenting as exfoliative erythroderma. J Am Acad Dermatol. 1998
Nov; 39(5 Pt 2): 827- 830.
6. Braun B, Baima B, Sticherling M. [Bullous pemphigoid
manifesting as dyshidrotic eczema and prurigo nodularis]. Hautarzt. 2002
Nov; 53(11): 739- 743.
7. Ross JS, McKee PH, Smith NP, Shimizu H, Griffiths WA,
Bhogal BS, et al. Unusual variants of pemphigoid: from pruritus to pemphigoid
nodularis. J Cutan Pathol. 1992 Jun; 19(3): 212- 216.
8. Geiss Steiner J, Trueb RM, Kerl K, Muhleisen B, French
LE, Hofbauer GF. Ecthyma-gangrenosum-like bullous pemphigoid. Dermatology.
2010; 221(2): 142- 148.
© 2011 Egyptian Dermatology Online Journal
|




