|
|
Summary
Systemic lupus erythematosus (SLE) is known to
present with diverse clinical features. The disease has a predilection
for females. Here, we report a case of SLE in a male patient
masquerading as pyrexia of unknown origin and culminating in multi-organ
failure. The case is being reported for its unusual presentation and
rarity in male gender. High index of suspicion is required for early
diagnosis of the disease so as to avoid delay in initiation of treatment
and minimise mortality associated with the illness.
Introduction
SLE like most other autoimmune diseases has a
predilection for female sex. The disease is characterised by the
development of auto-antibodies directed against various body proteins.
The disease can have a vague presentation at least initially which may
result in delay in the diagnosis and an adverse impact on the prognosis.
Here, a case of SLE in a male is being reported for its unusual
presentation which probably led to the delay in diagnosis and poor
outcome of the disease [1,2].
Case Report
Forty years old male, farmer by profession,
presented with complaint of fever for the last 3 months. Fever was low
grade, intermittent not associated with rigors or chills.
Moreover, there was history of easy fatigability,
malaise and myalgias.
On examination, patient had an oral temperature of
101o F with non- inflammatory and non- scarring patchy alopecia of scalp
(fig. 1).
The patient also had significant cervical and axillary lymphadenopathy.
Lymph nodes were soft, discrete, non-tender and not adherent to the
underlying tissue or skin. The rest of the systemic examination was
unremarkable.
Investigations of the patient revealed normocytic,
normochromic anemia with normal total leucocyte and platelet count.
However he had high ESR (37mm) and transaminitis.
Other routine investigations including kidney
function test, fasting blood glucose, serum electrolytes, spot urine
examination, chest skiagram and USG abdomen were normal. Retro viral
serology was nonreactive. Axillary lymph node excision biopsy revealed
non-specific lymphadenitis. CT chest did not reveal any adenopathy. A
workup for chronic infections especially common in this region like
tuberculosis and brucellosis was unrewarding.
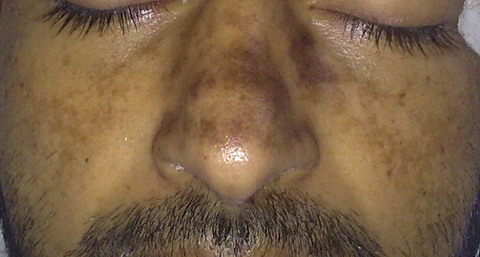
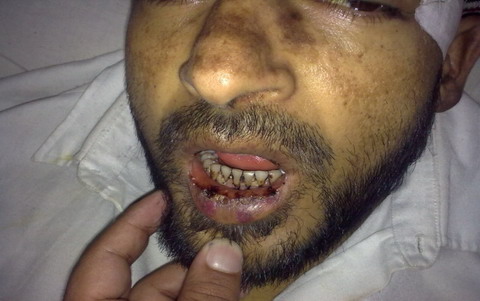
During hospital stay, patient developed malar rash
with oral ulceration (fig. 2-3).
This was followed by pancytopenia. At this stage
ANA & anti-ds DNA were positive in high titres by immuno-florescence.
Subsequently patient developed epistaxis followed by bleeding from lymph
node biopsy site and melena. Serum creatinine and blood urea of the
patient started to rise. There was further decline in platelet count to
1000/mm3. It is pertinent to mention here that he maintained normal
sensorium till end thereby negating the diagnosis of thrombotic
thrombocytopenic purpura. With aforementioned clinical and laboratory
sequence of events, a diagnosis of systemic lupus erythematosis
masquerading as pyrexia of unknown origin and culminating in multi-organ
failure was contemplated as he was fulfilling requisite criteria for the
same [3].
Patient was put on methyl prednisolone 1gm/day pulse therapy. However
patient's condition continued to worsen despite requisite therapy.
Finally patient developed hemodynamic compromise, multi-organ failure
and succumbed to the disease.
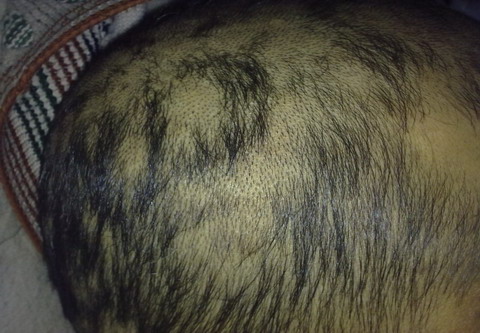
| Fig 1: Non scarring alopecia of scalp. |
|
Discussion
Systemic lupus erythematosus (SLE) is a
multi-organ system autoimmune disease with numerous immunological and
clinical manifestations. It is characterized by an auto-antibody
response to nuclear and cytoplasmic antigens. The disease mainly
involves the skin, joints, kidneys, blood cells, and nervous system
Systemic lupus erythematosus (SLE) has traditionally been considered a
disease of women, and is uncommon in men. For all ages, the female to
male ratio is 7:1 and 11:1 during the childbearing years [4].
As a rare auto-immune disease of males, lupus is commonly misdiagnosed
or under-diagnosed leading to life impacting complications. The initial
clinical course of systemic lupus erythematosus (SLE) is variable,
ranging from relatively minor manifestations progressing over years to
rapid onset of fulminate.
Several studies have tried to characterize lupus
in men, in particular searching for any clinical differences between men
and women. SLE in males tends to occur at an earlier age than female
counterparts [5].
Male patients usually have a more severe disease, with higher morbidity,
specially related to renal disease [6].
Renal disease occurs with an increased frequency and is usually more
severe than females [6,7,8].
Moreover there is higher prevalence of serositis and thrombocytopenia [7,8,9].
However the prevalence of alopecia, arthralgia, Raynaud's phenomenon and
psychosis are lower than female patients [8].
Among the neurological manifestations, males have higher frequency of
seizures and peripheral neuropathy whereas females tend to have more
psychiatric symptoms and headache [5].
Male patients of African- American race are more
likely to have nephritis as their first clinical symptom and they
usually progress from initial clinical manifestations to SLE diagnosis
more rapidly than other ethnic or gender groups [10].
It has been seen that male SLE patients from India
have a higher incidence of mucocutaneous and renal involvement and a
lower incidence of neuropsychiatric, gastrointestinal and hematological
disease in comparison to those published from the developed countries.
Moreover higher frequency of infection, particularly tuberculosis, was
seen in male patients, which was the cause of death in some [5].
Potential causes of the female predilection for
SLE included the effects of estrogen and its hydroxylation, decreased
androgen levels, hyper-prolactinemia, and differences in
gonadotropin- releasing hormone (GnRH) [7].
In men and women with SLE and in their first-degree relatives estrone is
preferentially hydroxylated at the C-16 position, resulting in the
accumulation of 16-hydroxylated metabolites, which have sustained high
estrogenic activity.
Men and women with SLE might have too much
estrogenic and too little androgenic hormone, shifting their immune
system toward increased responses. Prolactin levels are elevated in some
individuals with SLE and may increase disease activity [11].
Conclusion
SLE can have bizarre clinical presentation. High
index of suspicion is needed to arrive at a proper diagnosis at the
earliest, especially in male sex, in order to minimise mortality
associated with the disease.
References
1. Epidemiology of Systemic Lupus Erythromatosis in a northern
Spanish population: gender and age influence on immunological factors. Lupus
2003; 12: 860- 865.
2. Mona H B, Enamul H, Hesham AA.Male Adolescent with Systemic
Lupus Erythromatosis.Kuwait Medical Journal 2007, 39(2): 181- 183.
3. Hochberg MC. Updating the American College of Rheumatology
revised criteria for the classification of systemic lupus erythematosus.
Arthritis Rheum. 1997; 40(9): 1725.
4. Manzi S. Epidemiology of systemic lupus erythematosus.
Am J Manag Care Oct 2001; 7(16 Suppl): S474- 479
5. Ira pande , A.N.Malaviya. SLE in Indian Men: Analysis
of the Clinical and Laboratory Features with a Review of the Literature.
Lupus 1994; (3): 181- 186.
6. L.T.L Costallat: Systemic lupus erythematosus in 18 Brazilian
males: Clinical and laboratory analysis. Clin rheumatology Dec 1993; 12(4):
522- 525.
7. MD Sherif, Z. Yacoub; Gender differences in systemic
lupus erythematosus. Gender Med Issue Aug 2004; 1; 12- 17.
8. Jitima Mongkoltanatus, Suparaporn Wangkaew, Nuntana Kasitanon
and Worawit Louthreno. Clinical features of Thai male lupus: an age-matched
controlled study. Rheumatology Int Feb 2008; 18 (4): 339- 344.
9. A. Oclay, Ines domenech: Systemic Lupus Erythematosus
in Males: Analysis of Clinical and Laboratory Features. Lupus 1992; 1 (5),
295- 298.
10. M R Arbuckle, J A James, G J Dennis, M V Rubertone
et al. Rapid clinical progression to diagnosis among African-American men
with systemic lupus erythematosus. Lupus 2003; 12(2), 99- 106.
11. Walker S.E., McMurray R.W., Houri J.M., et al: Effects
of prolactin in stimulating disease activity in systemic lupus erythematosus.
Ann N Y Acad Sci 1998; 840: 762-772.©
2010 Egyptian Dermatology Online Journal
|